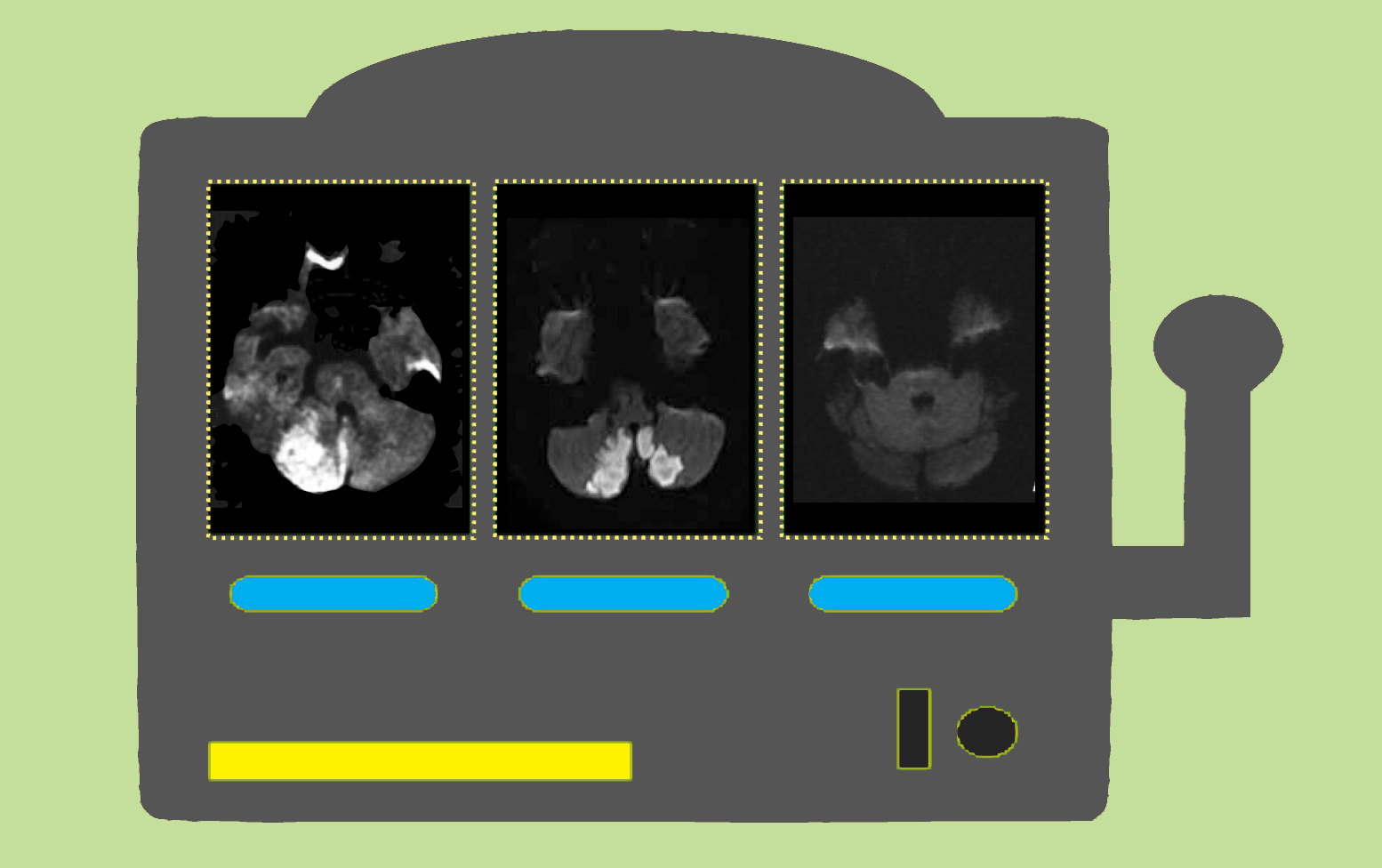
No Guarantees: MRI in the diagnosis of acute posterior stroke
Clinical scenario: An elderly male is brought in by EMS one evening after he developed sudden onset of vertigo 1 hr prior to arrival. He was watching a show when he suddenly felt that the world was spinning. On initial presentation, he had intermittent, unilateral nystagmus and was unable to walk on his own for unsteadiness and fear that he would fall. He had no other focal neurologic deficits or extremity ataxia. His NIHSS was 0. The physicians felt unsure about the diagnosis of acute posterior circulation stroke, so after discussion with the patient, a hyperacute MRI was performed and was negative. However, after returning fromMRI, the patient developed worsening nystagmus and agreed to received tPA despite negative imaging.
Clinical question: What is the sensitivity of DWI (Diffusion Weight Imaging) MRI for acute posterior circulation stroke and should this be used to help make decisions regarding tPA administration?
Literature Review: Posterior circulation strokes are notoriously difficult to diagnose. This is because their presentation is dominated by non-specific symptoms such as nausea/vomiting and dizziness as opposed to the more obvious neurologic presentations of weakness, numbness and slurred speech found with anterior circulation strokes. The NIHSS itself is strongly geared towards detecting deficits due to anterior circulation pathology. Probably because they are difficult to diagnose, posterior circulation strokes are also missed more often. In one recently published retrospective study of 465 patients seen at both academic and community centers, 37% of posterior circulation strokes were initially misdiagnosed compared to 16% of anterior strokes (p < 0.001) [1].
Failing to consider the diagnosis of posterior stroke is one etiology of missed diagnosis. In the above mentioned study, only 8% of missed strokes were triaged as stroke codes [1]. A fair number of missed strokes also were missing neurologic exams (18% at an academic hospital and 65% at a community hospital). Even when neurologic exams are charted, documentation (and by assumption) examination of neurologic findings associated with posterior circulation stroke (eye movements, coordination and gait) is often omitted [2]. But even when a full neurologic exam is performed, the diagnosis of posterior circulation stroke is not always crystal clear. As posterior circulation strokes can present more of a diagnostic dilemma, it would be nice if emergency physicians could rely on imaging to be more confident in the diagnosis of stroke (or lack thereof). This is especially true prior to discharging a patient home with an alternative diagnosis or administering tPA to a patient presenting within the treatment window. Unfortunately, such confidence may not be possible. Several studies have examined the false negative rate of DWI imaging in ischemic stroke and their results are far from comforting:
An initial study from the late 1990's retrospectively estimated the false negative rate of DWI imaging in ischemic stroke [3]. They evaluated the imaging of 139 patients who were admitted to a stroke center between 1998 to 1999 with signs and symptoms suggestive of arterial ischemic stroke and in whom symptoms persisted for at least 24 hours. All patients had initial MRI within the first 48 hours of presentation (93/139 within the first 24 hrs). All patients who had a negative initial MRI had a follow-up MRI prior to hospital discharge. The study identified 8 patients who initially had negative DWI imaging but had a positive MRI 8 to 70 hrs later. Significantly, 6 of 8 false negative MRIs were located in the posterior circulation, giving an overall false negative rate for posterior circulation CVA of 31%.
Another prospective study enrolled 401 patients with stroke symptoms between March 2002 and March 2005 [4]. All the patients had an MRI within 24 hrs of symptom onset and a follow-up MRI at 30 days. 103/401 patients (25.6%) had negative initial imaging. Of these 103 patients, 26 were eventually diagnosed with stroke at 30 days based on a combination of imaging and clinical data. The false negative rate for DWI in patients with a brain stem stroke location was 30%. DWI imaging also missed a large number of lacunar infarcts that were found on follow-up imaging.
These first two studies may be considered limited due to their age, as they are 16-17 years and 11-14 years old respectively. However, a more recently performed retrospective study found similar results. This study was performed at an institution where hyperacute MRI is incorporated into the tPA protocol [5]. The authors reviewed the records of 569 patients who received tPA from 2004 to 2010. 518 of these had a DWI lesion. Four turned out to be stroke mimics, including one which had a false-positive DWI lesion. The overall sensitivity of DWI for a stroke anywhere in the brain was 92%. Factors associated with having DWI-negative initial imaging included having a less severe stroke (NIHSS 4 vs. 7), a better outcome (% modified Rankin scale 0-1: 80.9% vs. 61.8%), a longer time to imaging (120 minutes vs. 109 minutes) and having a posterior circulation stroke. Indeed, DWI imaging was found to be negative in 34.9% patients with posterior circulation strokes.
So, is there anything better to than DWI imaging to help with this difficult diagnosis? Indeed there is, and it’s cheaper than an MRI. Studies of the HINTS exam (Head impulse test-nystagmus-test of skew) suggest that it outperforms MRI with a sensitivity of 100% and specificity of 86% for stroke in patients presenting with acute vestibular syndrome [6]. However, in this study, the test was performed by a neuro-ophthalmologist. The sensitivity and specificity of this bedside test when performed by emergency physicians is still to be determined [7].
Take home: DWI imaging will be negative in about a third of patients with acute posterior circulation stroke. Consideration for administration of tPA should be done of the basis of physical exam (HINTS), clinical gestalt and discussion of the risks and benefits with the patient.
Submitted by Maia Dorsett (@maiadorsett), PGY-4
Faculty Reviewed by Peter Panagos (@panagos_peter)
References:
1. Arch, A. E., Weisman, D. C., Coca, S., Nystrom, K. V., Wira, C. R., & Schindler, J. L. (2016). Missed Ischemic Stroke Diagnosis in the Emergency Department by Emergency Medicine and Neurology Services. Stroke, 47(3), 668-673.
2. Savitz, S. I., Caplan, L. R., & Edlow, J. A. (2007). Pitfalls in the diagnosis of cerebellar infarction. Academic emergency medicine, 14(1), 63-68.
3. Oppenheim, C., Stanescu, R., Dormont, D., Crozier, S., Marro, B., Samson, Y., ... & Marsault, C. (2000). False-negative diffusion-weighted MR findings in acute ischemic stroke. American Journal of Neuroradiology, 21(8), 1434-1440.
4. Sylaja, P. N., Coutts, S. B., Krol, A., Hill, M. D., Demchuk, A. M., & VISION Study Group. (2008). When to expect negative diffusion-weighted images in stroke and transient ischemic attack. Stroke, 39(6), 1898-1900.
5. Simonsen, C. Z., Madsen, M. H., Schmitz, M. L., Mikkelsen, I. K., Fisher, M., & Andersen, G. (2015). Sensitivity of diffusion-and perfusion-weighted imaging for diagnosing acute ischemic stroke is 97.5%. Stroke, 46(1), 98-101.
6. Kattah, J. C., Talkad, A. V., Wang, D. Z., Hsieh, Y. H., & Newman-Toker, D. E. (2009). HINTS to diagnose stroke in the acute vestibular syndrome three-step bedside oculomotor examination more sensitive than early MRI diffusion-weighted imaging.